Cervical Disc Replacement: What I Learned After 15 years & Hundreds of Cases
By Dr. Huffman
Cervical disc replacement is still a new form of spine surgery to many surgeons, but it has been a tried and true part of my surgical practice since I began. I participated in my first disc replacement surgery in 2004 during my spine surgery fellowship with Dr. Rick Delemarter and I made the procedure a mainstay of my practice when I started working in Napa in 2005. Since that time I have performed hundreds of disc replacements and I have learned a few things about the procedure. Over the past 15 years, numerous studies have come out demonstrating the benefits of cervical disc replacement over the “gold standard” of anterior cervical discectomy and fusion. For this blog, I wanted to take some time to discuss this spine surgery treatment option including an explanation of the reasons to consider disc surgery in the neck.
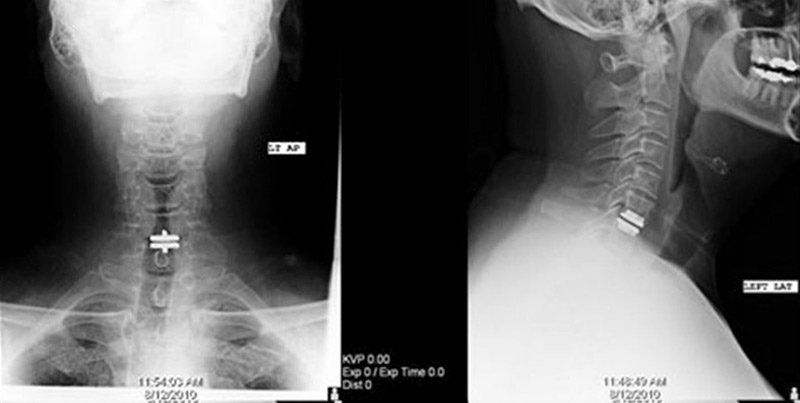
Photo: spine.org
When is Disc Surgery Needed?
Before getting into the details of surgery, there are three general indications for disc surgery in the neck: spinal cord compression, compression of a nerve root coming off the spinal cord by the disc, and painful disc disease.
Spinal Cord Compression. Out of the three indications, spinal cord compression is the strongest. This causes a condition known as myelopathy which describes a situation where compression of the spinal cord results in damage to the inside of the cord. The symptoms of this can be subtle and pain may often only be mild. The biggest thing people notice is loss of balance and loss of hand coordination. Sometimes I find out people are myelopathic when they have had a fall that a normal person should not have. What is confusing is that people often think they are just getting old and clumsy. The reason that myelopathy is so important to catch early is that these changes are irreversible. Once someone starts to develop symptoms of myelopathy and spinal cord compression is demonstrated, there is little role for non-operative treatment.
Spinal Nerve Root Compression. Spinal nerve root compression is different than spinal cord compression. The main symptoms of nerve root compression is pain and others include weakness or numbness. It is analogous to sciatica. Unlike spinal cord compression, the symptoms of nerve root compression can improve with time and are more commonly reversable with surgery. For this reason conservative care and time are usually given a chance before surgery is considered. When surgery is considered, the success rate, especially for relieving pain, is relatively high.
Neck Pain with Degenerative Disc Disease. The last reason to consider cervical disc surgery is neck pain with degenerative disc disease. Unfortunately surgery for this condition is not as successful and sometimes leads to increased pain. For this reason, conservative measures are exhausted before surgery is considered. Fortunately, this type of mechanical neck pain almost always responds well to conservative care.
The Standard Method: Anterior Cervical Discectomy & Fusion
In the case that cervical disc surgery is indicated, the historical “standard of care” has been to remove the disc from the front then “fuse” the bone above and below the disc together. Fuse means to make two bones grow together into one bone so there is no longer motion between the bones. The fusion technique has evolved from using a piece of bone from the hip area of the pelvis to using a plate and screws with donor bone. More recently surgeons have started using “cages” that have integrated fixation to hold them into the bone above and below the disc that has been removed. In all of these techniques the actual therapeutic part of the surgery is to remove the disc and bone spurs that are pinching the spinal cord or nerve roots and this part of the surgery works well. Once the pressure is off the pain of pinching the nerve or the damage to the spinal cord is stopped. Unfortunately if you stop there you have a hole in the front of the spine where the disc was which is what led surgeons to fuse these cases.
As mentioned, the initial success rate of fusion is high. In the neck studies have shown greater than 90% of patients have significant improvement in their symptoms following a one level cervical fusion.
There are two problems with fusions however.
First, there is a chance it does not fuse. For a single level case this chance is low but for multi-level cases it goes up considerably. The other problem is more long term. Basically if you take away motion from one level by fusing it together, the level above and bellow take up the strain and wear out more quickly which may ultimately lead to the need for additional surgery.
An Alternative Method: Cervical Disc Replacement Surgery
Disc replacement surgery starts out like a fusion surgery. The disc is removed from the front of the neck allowing decompression of the spinal cord and nerve roots. Then, instead of putting a bone graft or a cage between the bones and locking them together a disc replacement is placed. Like a knee replacement or a hip replacement the disc replacement moves. This allows the level which had the disc removed to move approximately like it would with a normal disc. There is no risk that the two bones do not fuse together and because it moves there is not additional strain placed on the disc above and below so they will wear at a normal rate and not an increased rate.
What does this really mean for disc replacements? Since the disc has been removed and the pressure is alleviated from the spinal cord or nerve root this procedure has a similar initial success as the fusion. There is no need to wait for fusion so recovery is also easier. Patients can start moving their neck right away and do not need to wear a restrictive and uncomfortable collar. Finally and probably most importantly, the rate of additional surgery is significantly lower with disc replacements than with fusions so long term patients are less likely to need another operation on their neck.
What about replacing more than one disc at a time?
If you think about it all the problems associated with a fusion, specifically the failure to fuse and the increased strain on the other levels of the neck, must get worse the more levels you fuse. It turns out this is true. The success rate of a two level fusion is not as good as that of a single level and three levels are even less successful. This is where disc replacement really shines. While studies suggest that single level disc replacements do a little better than single level fusions, for two level surgeries the difference is significantly greater. Logic suggests that this will be the case for three level disc replacement compared to fusion but this has not been well studied and is not currently FDA approved.
In my experience I have seen a fairly significant difference when I compare the outcomes of my disc replacement patients to those of my fusion patients. When the underlying condition is the same I have found that disc replacement patients recover faster and are less likely to return several years later with new problems at other levels in their neck. In addition I have not seen any complications directly due to a failure of the disc replacement.
What are the risks of disc replacement?
Well, no surgery is perfect and the outcome can never be completely predicted. There are many potential risks but these are the most common ones. Disc replacement involves a surgical exposure of the front of the neck where there are a number of things that can be injured including the arteries that supply blood to the brain, the esophagus which carries food from the mouth to the stomach and the nerves that work the vocal cords. Inside the spine itself there is a risk of injuring the spinal cord or the nerve roots. In addition like any surgery there is a risk of bleeding or infection. The surgery is done under a general anesthesia so you are totally asleep but there are also risks of general anesthesia including a bad reaction to the anesthesia and pneumonia. Fortunately the overall risk is low making this one of the most successful surgeries that I preform.
Who is a Candidate?
Lastly, every case is different and not everyone is a candidate for disc replacement surgery. Sometimes too much bone needs to be removed in order to adequately decompress the nerves and spinal cord making a fusion necessary. Other times the bone is not strong enough to support the disc replacement or there may be too much arthritis. And of course some insurance companies still do not pay for the procedure, calling it experimental even 14 years after it was FDA approved.
To find out more about disc replacement and to see if you are a candidate call for an appointment.
Read More Blog Posts:
Request An Appointment
Address: 3273 Claremont Way, Ste. 201, Napa, CA 94558
Phone: 707-603-1042
